chronic bilateral airspace opacification (differential).chronic unilateral airspace opacification (differential).acute airspace opacification with lymphadenopathy (differential).acute bilateral airspace opacification (differential).acute unilateral airspace opacification (differential).differential diagnoses of airspace opacification.differential of left paramediastinal catheter positions.peripherally inserted central catheters.evaluation of endotracheal tube position.evaluation of nasogastric tube position. 
Meanwhile, high flow rates have higher risk of catheter rupture with uncertain gurantee of image quality 4,5. Slow injection rate of 2ml s -1 only minimally compromise the image quality. Localizing the the position of CVC before and after the injection Safety protocols when using CVC as intravenous contrast injection site are 5:Īspirating blood before the injection of contrast media Automatic power injection or hand injection of contrast media poses the same risk of catheter rupture 4. Among the complications are 4:Ĭatheter rupture leading to contrast extravasationĬatheters more than 3 months old have increased risk of rupture. Guidewire shearing and fragment embolizationĬontrast injection through a central venous catheter is safe with complication rate of 1% if a strict protocol is followed. Ultrasound-guided CVL insertion is proposed to reduce the number of complications and to increase the safety and quality of central venous catheter (CVC) placement. There is a limited differential of left paramediastinal catheter positions. Policy varies by institution but tip placement for neck/thoracic/upper limb CVCs in the superior vena cava or at the cavoatrial junction is generally acceptable. Internal jugular vein (see: jugular venous catheters)įemoral vein (typically only short-term access)īrachial, basilic or cephalic veins (for PICCs and implantable ports) May be located in the chest or arm (brachial)Ĭentral venous catheters can be inserted into a variety of veins, most commonly including: Hickman catheters, Groshong catheter, Broviac line, Permcath Vascath is used for haemodialysis, apheresis, stem cell collection, etc.Į.g. used in ICU or ED for emergent or short-term (<7-10 days) accessĮ.g. Peripherally inserted central catheters (PICC)Į.g. There are other agents to use on some of the lipid and mineral precipitates. So always get a quick hx of what has been given.so if they were using it for Dilantin and then suddenly its occluded.odds are its a precipitate and NOT a thrombotic occlusion. Remember Tpa will not work for any occlusions caused by a precipitation. Current literature and studies indicate the link between thrombotic occlusions (complete or partial) and an elevated risk of infection. 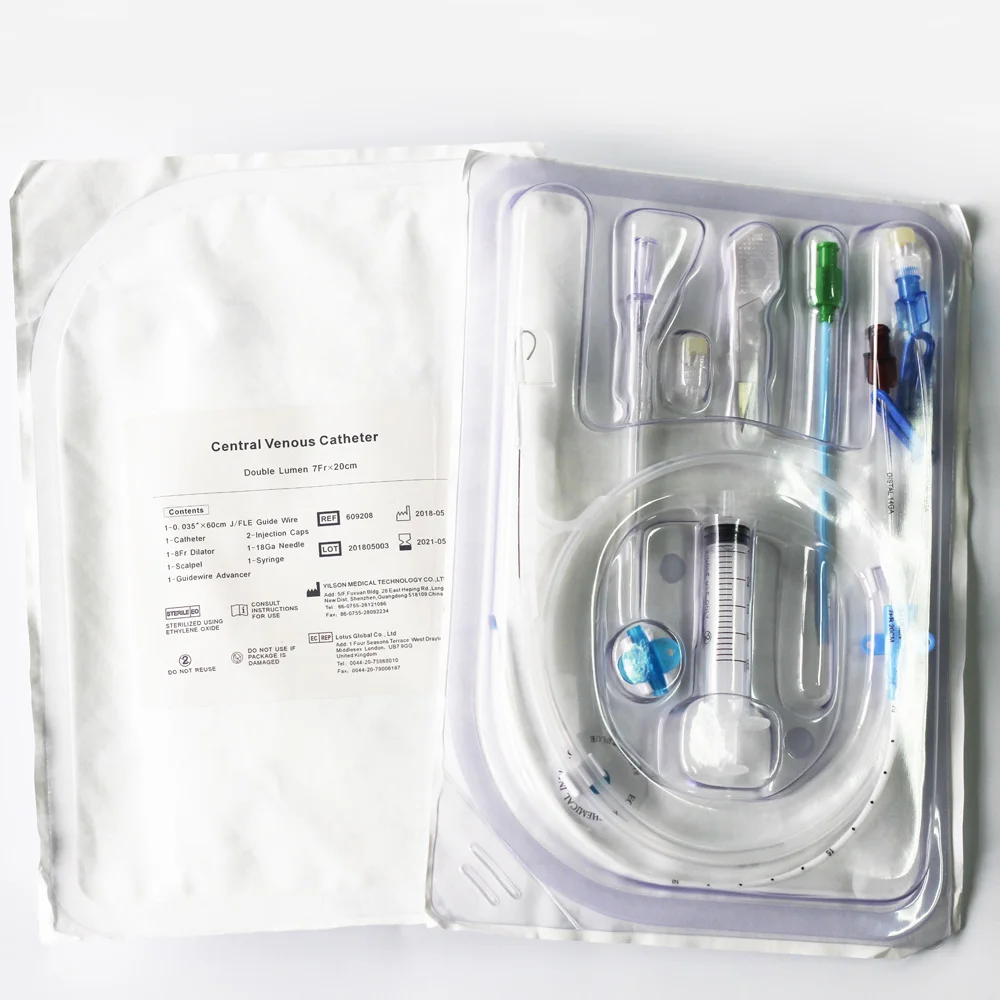
On occasion I will not not treat a PWO on a percutaneously placed CVC if I know for certain it is coming out tomorrow. The trend is going to a zero tolerance on all CVCs, So we must do all the things that help us achieve very low or non existent catheter related bloodstream infections. What brand and name of NS are you using? There is a whole new technology to catheter flushing now and you need to look at the VAD as a whole unit to include the catheter the valve type and flushing procedures and flush type. There are special NS prefills on the market that are specifically made to reduce reflux into the distal end of any CVC (all kinds of course). If it is happening a lot you need to look at your flushing protocols, the types of LAD you are using and the type of prefill NS you are using. Yes, generally speaking these need to be treated. Yes the case you described is a persistent withdrawal occlusion (PWO) so you can easily instill but not easily withdraw or not at all. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
